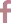- Home
- Trend
- Weight Loss Strategies
- Acne Tips
- Hair Health Information
- Blemish Removal Tips
- Acne Scar Removal Tips
- Muscle Building Techniques
- Intimate Care Tips
- Postpartum Intimate Care
- Eye Bags Wiki
- Tips for Face Slimming
- Secret of Permanent Hair Removal
- Breast Enlargement Tips
- Cure to Snoring
- Marionette Lines
- Skin-Tightening Secrets

免費體驗
Acne Treatment
1 Minute Self-Registration
Date should not be before minimal date
Acne is a widespread skin condition affecting millions globally, but within the realm of acne lies a distinct type often misunderstood and misdiagnosed—fungal acne. This comprehensive guide delves into the nuances of fungal acne, exploring its symptoms, causes, and, most importantly, effective treatments.
1
The Science Behind Fungal Acne: Why Traditional Acne Medications Won't Work

The persistent nature of some skin conditions, often mistaken for traditional acne, can be attributed to a phenomenon known as Fungal Acne or scientifically, Pityrosporum Folliculitis. This condition deviates from conventional acne, as it is not a result of bacterial factors but rather a yeast infection affecting hair follicles. The primary culprit behind Fungal Acne is a specific type of yeast called Malassezia. While Malassezia is typically present on the skin's surface, an overgrowth of this yeast, triggered by various factors, can lead to the development of Pityrosporum Folliculitis.
It is crucial to recognize that the term "fungal acne" is a misnomer; it is not a form of acne at all. Instead, it signifies a yeast infection occurring within the hair follicles. Unlike typical acne, which involves bacterial inflammation, Fungal Acne is characterised by the overproliferation of Malassezia yeast within the hair follicles. This overgrowth can result in a range of skin issues, including red and itchy bumps resembling acne lesions.
Malassezia, being a naturally occurring microorganism on the skin, particularly thrives in the environment of hair follicles, especially in conditions of high humidity. This tendency for overgrowth in specific conditions is a key factor in understanding why traditional acne medications may prove ineffective in treating Fungal Acne. Unlike bacterial acne, Fungal Acne requires a targeted approach that addresses the unique nature of yeast infections within the hair follicles. Therefore, understanding the science behind Fungal Acne and recognizing it as a distinct condition is essential for implementing effective skincare strategies tailored to its specific characteristics.

2
Watch Out the Symptoms of Fungal Acne

Watch Out for the Symptoms of Fungal Acne
Identifying fungal acne poses a challenge, as its symptoms often closely resemble those of traditional acne. However, crucial distinctions exist that can aid in accurate diagnosis and targeted treatment. Fungal acne typically presents as a series of uniform, itchy, and frequently pus-filled bumps. Recognizing these distinctive symptoms is imperative for effective management.
These symptoms can be further exacerbated by various factors, including compromised immune function, excessive humidity, and the use of specific medications. Understanding these root causes is essential for both managing and preventing the occurrence of fungal acne.
- Acne Stick: Clear Skin at Your Fingertips
- Can Pitted Acne Scars Heal Naturally? 3 Distinct Types + Complete Treatment Solutions
- What Causes Back Acne in Females? Discover The 8 Causes and 5 Major Solutions!
- What Does Period Breakouts Say About Your Body? Eastern & Western Remedies To Clear Hormonal Acne!
3
Why Do I Get These Fungal Infections?
The development of fungal acne is influenced by a combination of factors, and recognizing these elements is crucial for prevention. Here are several key contributors to the development of fungal acne:
Humidity and moisture
Fungal acne thrives in humid environments. Excessive moisture on the skin creates an ideal breeding ground for the yeast Malassezia, the culprit behind fungal acne.
Preventive Measures: Individuals living in humid climates or during hot seasons should prioritise keeping their skin dry. This may involve using absorbent powders, wearing breathable clothing, and showering promptly after sweating.
Compromised immune function
A weakened immune system can contribute to the overgrowth of Malassezia, making individuals more susceptible to fungal acne.
Preventive Measures: Maintaining a healthy lifestyle with proper nutrition, regular exercise, and sufficient sleep can bolster the immune system. Individuals with immune-compromising conditions should consult healthcare professionals for tailored advice.
Medication use
Certain medications, such as prolonged use of antibiotics or corticosteroids, can disrupt the balance of microorganisms on the skin, creating an environment conducive to fungal acne.
Preventive Measures: Individuals prescribed long-term medications should be aware of potential side effects. Dermatologists can offer guidance on skincare routines that help counteract the impact of these medications on the skin.
Occlusive skincare products
The use of occlusive skincare products, like heavy creams and oils, can trap moisture and heat on the skin, promoting the growth of Malassezia.
Preventive Measures: Opt for non-comedogenic and oil-free skincare products. Regularly cleanse the skin to remove excess oils and prevent the accumulation of potential triggers for fungal acne.
Prolonged sweating
Excessive sweating, especially in areas with friction, can create an environment favorable for fungal acne.
Preventive Measures: Practice good hygiene by showering after physical activities, wearing moisture-wicking clothing, and ensuring proper ventilation in areas prone to sweating.
Sharing personal items
Sharing items like towels, razors, or clothing can transfer the yeast responsible for fungal acne.
Preventive Measures: Avoid sharing personal items, especially in communal spaces like gyms or locker rooms. Maintain personal hygiene items separately.

4
The Difference between Traditional Acne & Fungal Acne

Distinguishing between acne vulgaris and fungal acne is essential for choosing the right treatment. Traditional acne responds well to antibacterial agents, while fungal acne requires antifungal interventions. A misdiagnosis could lead to ineffective treatment and a worsening of symptoms. Here are some key differences between fungal acne (pityrosporum folliculitis) and traditional acne:
1. What caused it
- Fungal Acne (Pityrosporum Folliculitis): Caused by an overgrowth of the yeast Malassezia. - Traditional Acne: Typically caused by the bacterium Propionibacterium acnes.
2. Appearance
- Fungal Acne: Often appears as small, itchy, uniform red bumps, and can be mistaken for traditional acne. It may be more likely to appear on the chest, back, and shoulders. - Traditional Acne: Characterised by a variety of lesions, including whiteheads, blackheads, papules, pustules, nodules, and cysts.
3. Triggers
- Fungal Acne: Can be triggered by factors that promote yeast overgrowth, such as humidity, sweat, and the use of occlusive skincare products. - Traditional Acne: Influenced by factors like hormonal changes, genetics, and the presence of excess oil (sebum).
4. Response to treatment
- Fungal Acne: Typically responds well to antifungal treatments, such as topical or oral antifungal medications. - Traditional Acne: May be treated with a variety of approaches, including topical or oral antibiotics, retinoids, and other acne medications.
5. Diagnosis
- Fungal Acne: Often diagnosed based on clinical appearance, response to antifungal treatments, and sometimes confirmed with skin scrapings for microscopic examination. - Traditional Acne: Diagnosed based on clinical appearance and history.

免費體驗
Acne Treatment
1 Minute Self-Registration
Date should not be before minimal date
5
What Can I Do If The Condition Gets Worse?

Neglecting or misdiagnosing fungal acne can lead to a worsening of symptoms. Initially, itchy bumps may evolve into more inflamed lesions, and the condition may spread if not promptly addressed. Early intervention and getting fungal acne treated is crucial to preventing the escalation of symptoms and ensuring a more effective treatment outcome.
Topical fungal acne treatment
Topical treatments are instrumental in the management of fungal acne, providing targeted relief by addressing the underlying yeast overgrowth. Antifungal creams and cleansers containing ingredients such as ketoconazole or pyrithione zinc have proven effective in reducing Malassezia proliferation and alleviating symptoms. Incorporating these products into a consistent skincare routine is essential for long-term management and improvement of the condition.
Skin scraping
In cases where the diagnosis is uncertain or further confirmation is required, dermatologists may perform skin scraping. This involves collecting a small sample of skin for microscopic examination, aiding in the identification of the yeast responsible for fungal acne. While this procedure may not be a routine part of treatment, it can be a valuable diagnostic tool to ensure accurate identification and targeted therapy.
Antifungal treatments
Both prescription and over-the-counter antifungal treatments are pivotal in addressing the issue. These medications are designed to specifically target the yeast overgrowth responsible for the condition, promoting skin healing. It's crucial to follow prescribed regimens meticulously and, if using over-the-counter products, to adhere to recommended usage guidelines.

6
Treat Fungal Acne with These Ways

Preventing fungal acne requires the adoption of effective skincare practices that focus on maintaining a healthy skin barrier and minimising conditions conducive to yeast overgrowth. Consistency is crucial in preventing future outbreaks. Adjusting your skincare routine to manage fungal acne involves incorporating practices that regulate sebum production and avoid contributing to excess oiliness. Here's a detailed guide on adjusting your skincare routine:
Choose Fungal Acne-Friendly Products
Selecting non-comedogenic skincare products is essential to prevent pore clogging. Opt for oil-free formulas in moisturisers and cleansers to avoid contributing to excess sebum on the skin.
Use Antifungal Cleansers
Look for cleansers containing antifungal agents such as ketoconazole, pyrithione zinc, or tea tree oil. Consistently cleanse affected areas, especially after sweating, to remove excess oil and prevent yeast overgrowth.
Gentle Exfoliation
Avoid harsh scrubs that can irritate the skin. Opt for gentle exfoliants like salicylic acid to unclog pores without causing inflammation.
Moisturise Appropriately
Use lightweight, non-comedogenic moisturisers to hydrate the skin without contributing to excessive oiliness. Avoid occlusive ingredients present in heavy creams that can trap moisture and heat.
Sun Protection
Choose non-comedogenic sunscreens to prevent pore blockage. Reapply sunscreen regularly, particularly if sweating or spending extended periods outdoors.
Avoid Irritating Ingredients
Eliminate products containing potential irritants such as fragrances and alcohol, as these can exacerbate inflammation.
Launder Personal Items
Regularly wash towels, pillowcases, and any fabric that comes into contact with your skin to minimise the risk of spreading the yeast.
Consider Prescription Treatments
Consult a dermatologist if over-the-counter treatments are ineffective. Dermatologists may prescribe stronger antifungal medications or other targeted therapies.
Monitor and Adjust
Observe how your skin responds to different products and adjust your routine accordingly. Regularly consult with a dermatologist to assess progress, discuss concerns, and make necessary adjustments to your skincare plan.
Individual responses to skincare products can vary, so it's essential to tailor these adjustments to your specific needs and preferences. If uncertain, consulting with a dermatologist can provide personalised guidance for effectively managing fungal acne.
- Acne Encyclopedia: Do Acne Emergency Remedies Actually Work?
- Expert Dermatologist Reveals The Best Ways To Treat Deep Acne Scars! Is Honeycomb Pico Laser Really Effective?
- Comedones: 4 Common Causes Of Blackheads And Whiteheads + Is An Acne Needle Effective?
- Should You Get An Exfoliating Gel For Silky Smooth Skin? 4 Key Benefits + Complete Buying Guide
7
Not Your Typical Acne Treatments: A Method to Prevent Future Fungal Acne Breakouts

The Acne Treatment from Perfect Medical plays a pivotal role in restoring smooth skin post-fungal acne recovery. This specialised treatment stands out by not only aiding in collagen production but also providing essential hydration, creating a robust defence against potential yeast attacks. Unlike invasive alternatives, this procedure offers a holistic approach, addressing various aspects of skin health.
One notable feature of the Acne Treatment is its capacity to remove dead skin cells through dual spiral suction and drainage technology. This not only enhances the immediate appearance of the skin but also serves as a preventive measure, reducing the likelihood of future pore blockages. The result is a clearer complexion with a reduced risk of recurring acne outbreaks.
As the treatment progresses, users can expect visible improvements in their skin's condition. This includes a significant reduction in acne breakouts, scars, and an overall enhancement of skin health. The skin appears brighter, fuller, and more hydrated, with a noticeable decrease in the unwanted oily sheen that often accompanies acne-prone skin.
A key component of the treatment involves the application of a medical-grade hydrating serum. This serum penetrates the innermost layers of the skin, providing deep hydration and nurturing the skin tissues. Simultaneously, it has a calming effect on sebaceous glands, helping to regulate oil secretion. The result is not only improved skin texture but also a decrease in the inflammation associated with acne.
Beyond its effectiveness, the Acne Treatment distinguishes itself by being a non-invasive option. It eliminates the need for surgery, incisions, injections, acne medication, or oral antibiotics. This makes the treatment suitable for a broad range of individuals, particularly those with moderate to severe acne, seeking a safe and comfortable solution.
Moreover, the procedure actively addresses acne scars through vacuum microdermabrasion, unclogging pores, relieving inflammation, and accelerating the healing process. This multi-faceted approach contributes to fewer acne breakouts and a significant reduction in the appearance of acne and blackheads.
Following the treatment, the commitment to personalised care continues. Our therapists offer professional and caring service, ensuring that each individual's unique needs are addressed. Through thorough follow-ups and a customised treatment plan, we aim to maximise the long-term benefits of the Acne Treatment, helping individuals achieve and maintain clear, smooth skin. Book a trial today to experience how the treatment can help you in soothing all kinds of traditional acne problems!

免費體驗
Acne Treatment
1 Minute Self-Registration
Date should not be before minimal date
FAQ

1. Is fungal acne contagious? Can I use traditional acne products for fungal acne?
Fungal acne is not contagious as it stems from an overgrowth of yeast on the skin and is not transmitted through person-to-person contact. Using traditional acne products designed for bacterial acne may exacerbate fungal acne. It is crucial to consult with a dermatologist to determine an appropriate course of action, which often involves using antifungal treatments specifically formulated for this condition. Seeking professional advice ensures an effective and targeted approach to managing fungal acne without causing further irritation.
2. Are there lifestyle changes that can help prevent fungal acne?
Yes, adopting good skincare practices is fundamental in preventing fungal acne. This includes regular cleansing, avoiding occlusive products that can trap moisture, and incorporating antifungal ingredients into your routine. Consistency in these practices is key to maintaining skin health and preventing future outbreaks of fungal acne. A dermatologist can provide personalised guidance based on individual skin needs.
3. Can stress trigger or worsen fungal acne?
While stress may not directly cause fungal acne, it can weaken the immune system, making individuals more susceptible to various skin issues, including fungal acne. Managing stress through relaxation techniques, adequate sleep, and a healthy lifestyle is beneficial for overall skin health. Combining stress management with a proper skincare routine can contribute to preventing and managing fungal acne effectively.
4. Is people with oily skin more prone to get fungal acne?
Individuals with oily skin are more prone to fungal acne due to the conducive environment created by excess sebum. Effectively managing oil production is crucial for both prevention and treatment. A targeted skincare routine designed to regulate sebum without excessively drying the skin is essential. Striking the right balance ensures skin health and minimises the risk of fungal acne flare-ups.
5. Can diet influence fungal acne?
Diet plays a role in fungal acne, with a diet high in sugar and refined carbohydrates potentially contributing to yeast overgrowth on the skin. Maintaining a balanced and nutritious diet, along with proper skin care practices, is vital for preventing and managing fungal acne. Consulting with a healthcare professional or dermatologist can provide personalised dietary recommendations to complement skin care efforts.